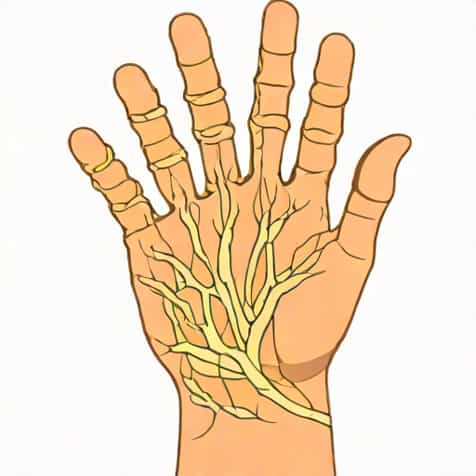
The ulnar nerve plays a critical role in the sensory and motor function of the upper limb, particularly the hand and forearm. Understanding its sensory distribution is essential for diagnosing nerve injuries, planning surgical interventions, and managing conditions such as neuropathy or compression syndromes. The ulnar nerve arises from the brachial plexus and travels down the arm, providing both motor and sensory innervation. Its sensory branches are responsible for transmitting sensations such as touch, pain, and temperature from specific regions of the hand and forearm to the brain. Knowledge of the ulnar nerve sensory distribution helps clinicians pinpoint the location and severity of nerve injuries and ensures accurate treatment and rehabilitation.
Anatomy of the Ulnar Nerve
The ulnar nerve originates from the medial cord of the brachial plexus, primarily carrying fibers from the C8 and T1 spinal nerves. It runs along the medial aspect of the arm, passes behind the medial epicondyle of the humerus, and continues into the forearm and hand. Along its course, it gives off branches that supply sensory and motor functions. Its unique pathway makes it susceptible to compression or injury, especially at the elbow (cubital tunnel) and wrist (Guyon’s canal). Understanding its sensory distribution is crucial for identifying clinical signs of ulnar nerve pathology.
Forearm Sensory Distribution
The ulnar nerve provides limited sensory innervation in the forearm, primarily through the dorsal cutaneous branch. This branch emerges in the distal forearm, supplying the skin on the dorsal and medial aspects of the hand and the proximal portions of the fourth and fifth fingers. Patients with ulnar nerve injury may report numbness or tingling in these areas, which can help localize the site of nerve compression or damage.
Hand Sensory Distribution
The ulnar nerve is most notable for its sensory supply to the hand. Its sensory branches are divided into the dorsal and palmar branches, each covering specific regions
Dorsal Branch
The dorsal branch of the ulnar nerve arises in the distal forearm, before the nerve enters the wrist. It supplies the dorsal aspect of the medial one and a half fingers (the little finger and half of the ring finger) and the corresponding portion of the dorsum of the hand. Sensory testing in this region is particularly useful for differentiating between proximal and distal lesions, as a lesion at the wrist may spare the dorsal branch while a lesion at the elbow would affect it.
Palmar Branch
The palmar branch of the ulnar nerve divides into the superficial and deep branches. The superficial branch provides sensation to the palmar side of the medial one and a half fingers, including the little finger and half of the ring finger. The deep branch, while primarily motor, contributes to sensation in certain areas of the hand, particularly the distal palmar regions near the fingers. Accurate mapping of the palmar sensory distribution is essential for assessing ulnar neuropathies and planning interventions.
Finger Sensory Innervation
The ulnar nerve is responsible for sensation in the medial aspect of the fourth finger (half of the ring finger) and the entire fifth finger. Both the dorsal and palmar surfaces of these fingers are innervated, with the dorsal surface mainly supplied by the dorsal branch and the palmar surface by the superficial palmar branch. Clinicians often test these areas to evaluate the integrity of the ulnar nerve following trauma, compression, or systemic conditions like diabetes that may affect peripheral nerves.
Clinical Relevance of Ulnar Nerve Sensory Distribution
Understanding the sensory distribution of the ulnar nerve is critical in clinical practice. It helps in diagnosing conditions such as cubital tunnel syndrome, Guyon’s canal syndrome, and ulnar neuropathy due to systemic illness. Patients may present with numbness, tingling, burning sensations, or pain in the regions supplied by the nerve. Mapping the affected areas allows healthcare providers to localize the site of injury or compression accurately.
Cubital Tunnel Syndrome
Cubital tunnel syndrome is a common condition resulting from compression of the ulnar nerve at the elbow. Sensory symptoms typically include numbness or tingling in the dorsal and palmar aspects of the little finger and medial half of the ring finger. Understanding the precise sensory distribution helps differentiate cubital tunnel syndrome from other nerve pathologies such as radial or median nerve compression.
Guyon’s Canal Syndrome
Compression of the ulnar nerve at the wrist within Guyon’s canal can lead to sensory deficits in the palmar aspect of the medial one and a half fingers, while sparing the dorsal branch. This distinction is important for diagnosis and highlights the relevance of knowing the ulnar nerve’s sensory distribution. Patients may also experience weakness in hand grip and difficulty with fine motor tasks due to associated motor branch involvement.
Peripheral Neuropathies
Systemic conditions such as diabetes, autoimmune disorders, or trauma can affect the ulnar nerve, causing sensory disturbances in its distribution areas. Clinicians use sensory mapping to assess the severity and progression of neuropathies. Early detection of changes in sensation can guide interventions and prevent long-term functional deficits.
Testing and Assessment
Evaluating the sensory distribution of the ulnar nerve involves several clinical tests. Common methods include
- Light touch or pinprick testing on the palmar and dorsal aspects of the little finger and medial half of the ring finger.
- Temperature sensation testing to detect subtle deficits.
- Two-point discrimination tests to evaluate fine sensory perception.
- Tinel’s sign over the cubital tunnel or Guyon’s canal to identify nerve irritation or compression.
Accurate assessment allows clinicians to differentiate ulnar nerve issues from other peripheral nerve disorders and plan appropriate treatments such as physical therapy, splinting, or surgical decompression.
The ulnar nerve’s sensory distribution is a vital aspect of upper limb function, encompassing specific areas of the forearm, hand, and fingers. The dorsal branch supplies the dorsum of the medial one and a half fingers, while the palmar branch covers the palmar surfaces of these same fingers. Knowledge of this distribution is crucial for diagnosing nerve injuries, planning interventions, and managing neuropathies. Proper sensory mapping and assessment help clinicians accurately localize ulnar nerve pathology, guide treatment decisions, and improve patient outcomes. Awareness of the ulnar nerve sensory distribution ensures effective evaluation and management of conditions that affect hand and forearm sensation.